| Title | Physical therapy in dogs: applications and benefits | |
| Author | Maira Formenton DVM | |
| Status of this article | 5 Removed | |
| Date | 24/01/2016 | |
| Jobs related | ||
| Small animal related | ||
| Large animal related | ||
| Equine related | ||
| Exotics related | ||
| Vetboss Employment related | ||
| Vetboss Business related | ||
| Vetboss Finance related | ||
| Vetboss Small animal related | ||
| Vetboss Large animal related | ||
| Vetboss Equine related | ||
| Vetboss Exotics related | ||
| Content | Physical therapy in dogs: applications and benefits
Introduction Physical therapy is a science, a treatment method which includes a variety of different techniques that encompass biomechanical, physical and physiological concepts to promote health or prevent disease. It covers everything from the simplest aspects, such as proper movement, through to rehabilitation and pain control, with the focus on the patient's well-being at all times. To rehabilitate, in its broadest sense, means “to re-establish or restore former abilities such as character, reputation or condition”. Rehabilitation and physical therapy go hand-in-hand, aiming to return an affected system to working order, so the main goal of physical therapy is to improve or maintain the quality of a patient's life. Different goals are set for each patient, depending on the pathology or dysfunction present.
What are the indications of physical therapy? Pain relief is one of the main benefits of physical therapy. Pain, whether acute or chronic, can cause immunosuppression, loss of appetite, and malnutrition (pain is related to stress, which influences the ability to metabolize carbohydrates, proteins and fat, and decreases food consumption), and can lead to loss of limb use and consequent muscular atrophy, thus directly interfering with a patient's well-being. Pain alleviation can often be very challenging. Reducing inflammation decreases recovery time, and is often associated with pain control. Osteoarthropathies are typical of pathologies that cause a pain-inflammation cycle that leads many human patients to turn to physical therapy. Physical therapy may also permit a reduction in the use of analgesics and anti-inflammatories, which can cause problems with chronic use. In many cases physical therapy can prevent or minimize muscle atrophy; for patients with paralysis or paresis this is a fundamental goal in rehabilitation. Post-operative rehabilitation endeavors to eliminate or reduce after-effects, such as pain and inflammation, and to preserve unaffected joints, assist bone regeneration and perhaps allow a reduction in medication. Finally, physical therapy can be used to improve a patient’s overall physical condition, including weight loss, cardiovascular condition and physical conditioning. Some examples where physical therapy can be beneficial: •Treatment (or prevention) of back problems, such as intervertebral disc herniations, vertebral spondylitis/spondylosis, disc ankyloses and calcifications, and paresis and para/quadriplegia. •Diverse osteoarthropathies (e.g. coxofemoral dysplasia), assisting pain control and minimizing inflammation to allow better range of movement and muscular strengthening. •Post-operative care after orthopedic and neurological surgeries, such as cruciate ligament rupture, patellar luxation, meniscopathies, spinal surgery and fracture repair. •Geriatric care, where therapy can add to both life quality and duration, providing comfort and relief from chronic pain, leaving the animal more inclined to interact with its owner. •Limb asymmetry, muscular atrophies and contractions, and general joint stiffness, assisting restoration of limb function. •Increased or improved performance of competition animals, prevention and treatment of injuries. •Obesity, in conjunction with weight loss programs employing reduced calorie diets and exercise regimes.
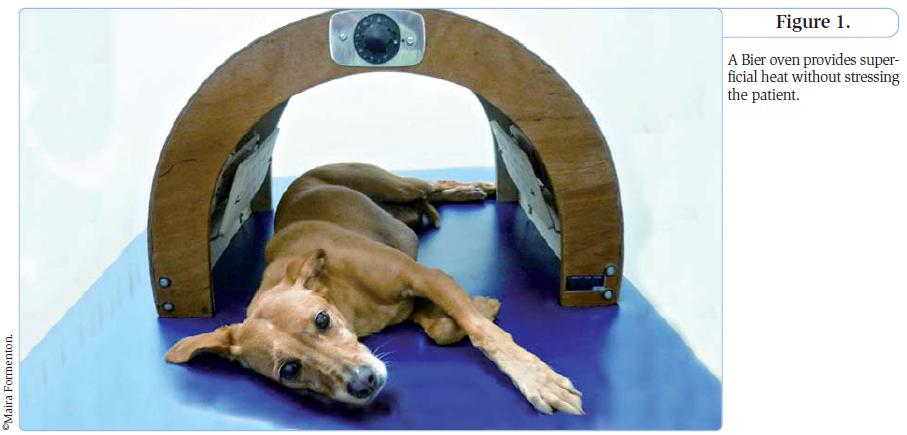
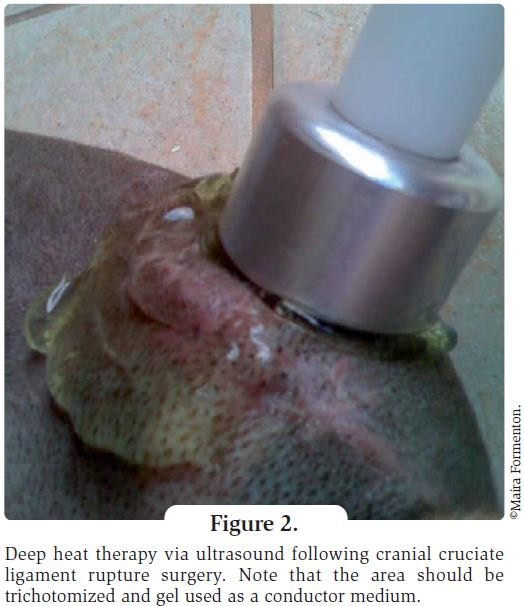
Main techniques used Thermotherapy Cold: cryotherapy is a simple and very effective method to control acute inflammation. Following orthopedic surgery icepacks may be applied to the surgical site for 20 minutes every 6 hours, for up to 48-72 hours. This also helps in pain control, but it should be avoided with chronic pain and inflammation (1). Heat: thermotherapy can be divided into superficial and deep techniques. Superficial heat methods include infrared lamps, hot water bottles, and hot compresses, as well as custom-built devices such as the Bier oven (Figure 1); these methods will achieve 1-10 mm depth of effective heating (1). Superficial heat is useful when treating chronic pain and is widely used for back problems. It can also facilitate therapy in cases of muscular contractions and joint stiffness. Heat should be applied for 20 minutes but is contraindicated for acute inflammation or if there are skin lesions at the application site (1). This therapy can often be performed by the owner at home with their animal as it is a simple and safe method. The primary deep-heat application method is ultrasound, using a high-frequency (17,000 Hz) transducer to produce vibration and hence heat within tissues (2). Deep heat can be very beneficial, reducing muscular spasms and contractions, increasing local blood flow, and reducing joint stiffness; the analgesic effect of the heat is also valuable. In chronic cases it can be used to reactivate the inflammatory process if indicated for treatment. Ultrasound also has athermic effects which can accelerate the healing processes for soft tissue and bone (2). Note it should not be used in malignant neoplasms or around the heart or eyes. It may be used with caution around the uterus in pregnant animals to treat acute inflammations (2) but should be avoided with orthopaedic implants, not because of the heat, but because ultrasound waves reflected from the implant can generate tissue damage. The dosage and application time is dependent on the depth of the target tissue and the area to be treated. Ultrasound is an excellent tool after orthopedic intervention, e.g. following cruciate ligament surgery where it aids the stifle to achieve better range of movement (Figure 2).
Massage therapy Massage is a very useful technique for veterinary physical therapy. The pain-tension-pain cycle is one of the key indicators for massage, especially for back problems, and is commonly used as part of the clinical routine. Massage decreases muscle tension, reducing pain and thus breaking the cycle. It also increases local blood flow, providing better tissue oxygenation and promoting removal of metabolic residues (due to better venous and lymphatic drainage) which assists return of muscle function. Better circulation also leads to an increase in the local temperature and muscular elasticity, accelerating tissue recovery. In many cases, muscular problems are associated with muscle contractions and adhesions that can be broken down with massage (Figure 3). There are few contraindications for this technique, but it should be avoided in patients with vascular problems, thromboses and clotting disorders, and malignant neoplasms, or where there are skin lesions and infection. Finally massage also releases endorphins, which lends the technique a natural relaxant effect (3). Kinesiotherapy Kinesiotherapy is treatment through movement. It may be passive (performed by the therapist), active (performed by the patient) or assisted (performed by the patient with the therapist's assistance) (4,5). The technique is considered one of the most important parts of the rehabilitation process. Guided therapeutic exercises and movements enable impaired systems to return to function, and can be invaluable in certain cases, e.g. rehabilitating the paralyzed patient with a herniated disc. Worth mentioning among the techniques are stretching, tractioning, and assisted movements, which include isometric, isokinetic and isotonic exercises (Figure 4). Kinesiotherapy can also promote beneficial self-awareness. Simple procedures such as brushing an animal will stimulate the nervous system (4,5).
Electrostimulation Electrostimulation involves the use of devices that generate an electrical current, producing analgesia, relaxation and muscular strengthening. Among various systems, the most commonly used methods in the veterinary sphere are TENS and NMES (6). TENS (Transcutaneous Electrical Nerve Stimulation) promotes analgesia through neuromodulation by releasing endorphins and encephalins; it also directly inhibits hyper-excited sensory nerves. The analgesia provided by TENS supports the gate control theory of pain perception, which suggests that neurotransmitters released in electrotherapy block the transmission of painful passages by competition (6,7). TENS can be applied as two modes: •Conventional mode (frequency 40-150 Hz, current up to 30 mA, with 50-250 μs of pulse duration), where the analgesia is immediate but short-lived. The minimum application time is 20 minutes. •Burst mode, where analgesia is less immediate, but longer-lasting (up to 8 hours). It requires a higher intensity, which restricts its application in more sensitive animals. The same is true for TENS acupuncture, where analgesia commences some 30 minutes after application but can last up to 6 hours (6,7). NMES (Neuromuscular Electrical Stimulation) stimulates muscular contraction, aiming to reduce atrophy and aid muscle function return, and is useful for neurological and orthopedic rehabilitation. Using a frequency of ~40 Hz, with variable pulse duration (typically 250-300 μs) and intensity (6,7), several electrodes are usually employed and trichotomization (three-way application) of the area is recommended for best results. Note a water-based gel is necessary if silicone electrodes are utilized. Electrotherapy, whether for pain, or muscle relaxation, contraction or strengthening, is widely used and can help a patient immensely. Laser therapy LASER (Light Amplification by Stimulated Emission of Radiation) therapy is indicated in many situations. A laser emits an invisible beam of light with specific characteristics. When the photon beam penetrates tissue, it initiates different stimulatory or inhibitory biological reactions, thus acting in a biomodulatory way (8). The laser can increase cellular metabolism and multiplication (by accelerating the mitosis process), mediates local inflammatory factors and stimulates collagen production, ossification and neovascularization of tissues (9). It also causes release of endorphins and encephalins to relieve pain. It is useful for tissue healing and regeneration and is widely used in cutaneous lesions, pressure sores and scars, osteopathies, herniated discs and back pain, as well as encouraging neuron repair in peripheral nerve damage and ossification in fractures (8,9). The laser head should be held perpendicular to the contact surface (Figure 5). Dosage and wavelength varies according to the desired effect. Contraindications for laser therapy include animals with neoplasia, and the beam should avoid eyes (to avoid retinal damage), epiphyseal plates, sympathetic ganglia, areas of hemorrhage, the gonads and the pregnant uterus (8).
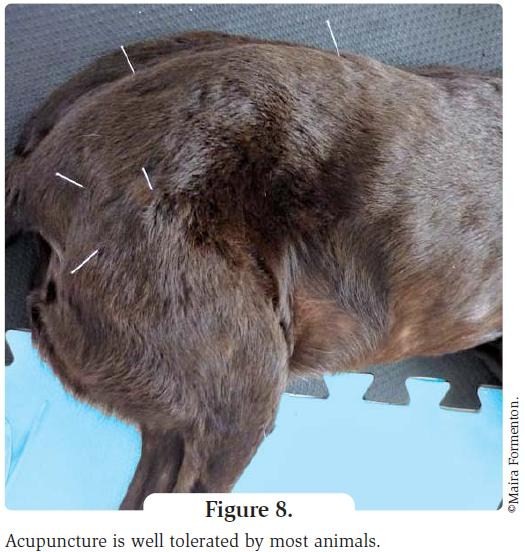
Hydrotherapy Hydrotherapy is the use of water as a treatment therapy. For animals, the forms that are usually applicable are swimming and the aquatic treadmill. This technique promotes many beneficial effects, both physiological and psychological. The advantages are obtained because the animal's weight and the exercise impact are reduced in the water. Hydrotherapy promotes better blood circulation, pain reduction, and increased flexibility and mobility; it strengthens muscle tone and even aids improvement in balance, co-ordination and posture maintenance. An animal with rear limb paralysis, for example, gains mobility in the water and can perform various exercises that would be impossible on solid ground. Moreover, water also works as an ideal sensory and selfperceptive stimulus that perfectly complements a patient's rehabilitation (10,11). If the water is heated this promotes muscular relaxation, increases circulation and improves lymph drainage, helping animals with edema, muscular contractions and spasms, and enabling pain relief and overall relaxation. Exercise in water also assists correction of improper posture, use of atrophied limbs and muscle and ligament strengthening, combined with a gain in muscle mass. The psychological effects cannot be disregarded; pain relief alone promotes wellbeing and improved quality of life, but the mobility that the animal gains in water helps it recover confidence and independence, which are often needed in order to start walking again. In many cases, an animal afraid to move due to psychological trauma gains a feeling of comfort from hydrotherapy and has the confidence to move an injured limb (10). An animal tends to use its front limbs strenuously when swimming, and this can therefore be the best option with forelimb injury. An aquatic treadmill is preferred for hindlimb injury and neurological rehabilitation. Water depth directly influences the therapy, as the greater the depth, the less the animal's weight. If the water is at the height of the greater trochanter of the femur, just 38% of the weight load is maintained (Figure 6), compared to 91% at tarsal level (11). Initially hydrotherapy should be for only a few minutes, just placing the animal in water to allow acclimatization. Once confidence is gained, therapy can commence, up to 20 minutes on a treadmill and 30 minutes swimming. Precautions include being wary of wounds, otitis, dermatopathies, and severe systemic disorders, especially cardiopathies, hepatopathies, kidney disease, and hyper- or hypotension. Uncontrolled epilepsy and respiratory conditions should also be evaluated (10). Finally, hydrotherapy can be used as an artifice to promote weight loss and physical conditioning for the animal. Calorie loss is considerable; for a weight loss and strengthening program, two or three times a week is recommended (Figure 7). Acupuncture Acupuncture is defined as the insertion of needles in pre-establi Note that the acupuncture sessions should preferably not be conducted at the same time as physical therapies. Aside from the prolonged session time, which can leave some animals impatient, laser therapy can interfere with acupuncture if applied at the same site, reducing its effect. Alternating treatment days is recommended.
Conclusion The use of different physical therapy techniques, whether by means of equipment or simple manipulation, generates excellent results and should therefore be considered and indicated as a treatment option for many orthopedic and neurological problems. A combination of techniques is often worthwhile, especially when physical therapy is used along with acupuncture, and can offer an animal the quickest and most favorable opportunity for rehabilitation.
This article was kindly provided by Royal Canin, makers of Mobility diet for dogs and cats. For the full range please visit www.RoyalCanin.co.uk or speak to your Veterinary Business Manager:
REFERENCES 1. Heinrichs K. Superficial thermal modalities. In: Millis DL, Levine D, Taylor RA, eds. Canine rehabilitation and physical therapy. Philadelphia: Saunders, 2004;277-288. 2. Hynynen K, Deyoung D. Temperature elevation at muscle-bone interface during scanned, focused ultrasound hyperthermia. Int J Hyperthermia, 1988;3:267-279. 3. Plews-Ogan M, Owens JE, Goodman M, et al. A pilot study evaluating mindfulness-based stress reduction and massage for the management of chronic pain. J Gen Int Med, 2005:20:12;1136-1138. 4. Amaral AB, Cinesioterapia. In: Mikail S, Pedro CR, eds. Fisioterapia veterinária. São Paulo: Manole, 2006;50-62. 5. Millis DL, Lewelling A, Hamilton S. Range-of-motion and stretching exercises. In: Millis DL, Levine D, Taylor RA, eds. Canine rehabilitation and physical therapy. Philadelphia: Saunders, 2004;228-243. 6. Mikail S. Eletroterapia. In: Mikail S, Pedro CR, eds. Fisioterapia veterinária. São Paulo: Manole, 2006;96-102. 7. Johnson J, Levine D. Electrical stimulation. In: Millis DL, Levine D, Taylor RA, eds. Canine rehabilitation and physical therapy. Philadelphia: Saunders, 2004;289-301. 8. Mikail, S. Laser Terapêutico. In: Mikail S, Pedro CR, eds. Fisioterapia veterinária. São Paulo: Manole,2006;81-90. 9. Tuner J, Hode L. The laser therapy handbook. Grängesberg, Prima Books, 2004;589. 10. Monk M. Hydrotherapy In: McGowan CM, Goff L, Stubbs N, eds. Animal physiotherapy assessment, treatment and rehabilitation of animals. 1st Ed. Oxford, Blackwell, 2007;187-197. 11. Levine D, Tragauler V, Millis DL. Percentage of normal weight bearing during partial immersion at various depths in dogs. In: Proceedings 2nd International symposium on rehabilitation and physical therapy in veterinary medicine. Knoxville, Tenn, 2002;189-190. 12. Shoen AM. Acupuntura veterinária: da arte antiga a medicina moderna. 2nd ed. São Paulo: Roca, 2006;190-195,707. 13. Maciocia G. Os fundamentos da medicina Chinesa: Um texto abrangente para acupunturistas e fitoterapeutas. São Paulo: Roca,1996;658. 14. Xie H, Preast V. Xie's veterinary acupuncture. Oxford: Blackwell, 2007;376. |
|
|
vetgrad.com is committed to handling personal data responsibly. Please view our Data Protection Policy |







 shed locations (Figure 8), producing various local and systemic physiological effects. For domestic pets there are 112 catalogued acupuncture points, and stimulation of certain points or a combination of points can cause different effects upon the organ/pathology to be treated (12,13). Acupuncture can achieve much faster and more effective pain control than through physical therapy alone; combining the two techniques is often very beneficial. The author recommends acupuncture in orthopedic/ neurological cases from the beginning of treatment, for cases such as peripheral and central vestibulopathies, disc herniations, and paresis/ paralysis. It is also useful for control of acute and chronic inflammation, (e.g. as a adjunct to treatment of arthropathies) and to control pain. It may be performed up to 24 hours before another physical therapy is initiated to facilitate the application of the technique. Additionally acupuncture has been described for the chronic effects of distemper, where it can help in the control of myoclonic movements and convulsions, and for neuropathic pain and peripheral nerve damage (12-14).
shed locations (Figure 8), producing various local and systemic physiological effects. For domestic pets there are 112 catalogued acupuncture points, and stimulation of certain points or a combination of points can cause different effects upon the organ/pathology to be treated (12,13). Acupuncture can achieve much faster and more effective pain control than through physical therapy alone; combining the two techniques is often very beneficial. The author recommends acupuncture in orthopedic/ neurological cases from the beginning of treatment, for cases such as peripheral and central vestibulopathies, disc herniations, and paresis/ paralysis. It is also useful for control of acute and chronic inflammation, (e.g. as a adjunct to treatment of arthropathies) and to control pain. It may be performed up to 24 hours before another physical therapy is initiated to facilitate the application of the technique. Additionally acupuncture has been described for the chronic effects of distemper, where it can help in the control of myoclonic movements and convulsions, and for neuropathic pain and peripheral nerve damage (12-14).