Show all small animal articles
Management of Liver Disease
James Kyffin BVSc (Hons) MRCVS - 29/09/2012
Management of Liver Disease
The liver plays a central role in many body processes including:
- Carbohydrate, lipid and protein metabolism (including clotting factors)
- Detoxification of metabolites and xenobiotics
- Storage of glycogen, fat, vitamins and trace elements
- Fat digestion
- Immunoregulation
The spectrum of clinical signs, clinicopathological and physical findings result from the deficiencies of these functions. The liver does have a large reserve capacity to perform these functions; up to 70% of liver mass can be lost before there is evidence of liver dysfunction.
Two groups of animals to investigate:
- Animal has persistently raised liver enzymes with no clinical signs; does it have liver disease?
- The animal has clinical signs; could it be liver disease?
Clinical Signs
Early clinical signs associated with liver disease can be quite vague and non-specific. Specific liver signs occur when reserves are used up; usually late in the disease but signs can be acute onset if severe pathology is present.

The clinical signs associated with hepatobiliary disease are typically referable to the GI, renal, neurologic or haematopoietic systems. In addition, dogs with chronic liver disease can develop hepatocutaneous syndrome, they develop a superficial necrolytic dermatitis of the face and distal extremities. Chronic hepatic diseases predisposes dogs to gastroduodenal ulceration, this can in part be due to portal hypertension, and this can cause associated clinical signs such as meleana, haematemesis, abdominal pain or a regenerative anaemia.
Hepatoencephalopathy (HE) develops when the liver is unable to detoxify inhibitory neurotoxins that are generated in the intestinal tract, one of these substances being Ammonia. The clinical signs are those of diffuse cerebral disease. HE is seen in cases with portosystemic shunts, either primary, congenital shunts or acquired shunts secondary to hepatopathies. It can also be seen in acute, fulminant hepatic failure. The signs associated with HE include disorientation, personality change, irritability, aggression, stupor, coma or seizures.

Ascites can develop with chronic hepatic disease, especially in the dog, and can signify primary or metastatic hepatobiliary disease, it can also occur in the form of bile peritonitis in cases of bile duct rupture. Ascites can be associated with the development of portal hypertension or hypoalbuminaemia.
A highly variable, but often predominant, early clinical sign in many dogs and cats with chronic hepatobiliary disease or PSS is the presence of polyuria and/or polydipsia. The aetiology behind this is unknown but several theories have been postulated:
- Psychogenic polydipsia
- Alterations in portal vein osmoreceptors
- Decreased hepatic urea production, resulting in disruption of renal medullary concentration gradient
- Potassium depletion
- Stimulation of thirst centre due to HE
- Increased endogenous cortisol levels associated with increased adrenal production or decreased hepatic degradation
Animals with hepatobiliary disease can develop clinical signs associated with ammonium biurate urolithiasis such as stranguria, pollakiuria or haematuria. Ammonium biurate stones form due to chronic hyperammonaemia and decreased hepatic processing of uric acid.
The most significant finding that can be associated with hepatic disease is icterus or jaundice. This results from accumulation of bilirubin and causes yellow discolouration of tissue, most readily apparent at the sclera and mucous membranes. Icterus can be pre-hepatic, hepatic or post-hepatic.
Diagnosis
Following a complete physical examination and taking a thorough history from the owner, a diagnosis of hepatobiliary disease may be expected. The diagnostic process usually involves:
- Blood samples (Biochemistry, haematology, bile acid stimulation test)
- Urinalysis
- Diagnostic Imaging
- Liver biopsy
Increases in the serum concentration of hepatic enzymes occur after hepatobiliary injury. These include alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatise (ALP) and gamma-glutamyl transpeptidase (GGT). These serum enzymes have a high sensitivity but poor specificity. The central role of the liver in metabolism and its high blood flow make it uniquely sensitive to secondary injury. Serum hepatic enzymes can be increased with any of the following:

The magnitude of the enzyme elevation is usually proportional to the magnitude of the hepatobiliary injury, however it is not predictive of the functional capacity of the liver (i.e., it is a measure of liver damage, not liver function).
Due to the regenerative ability of the liver, the degree of enzyme elevation is not indicative of prognosis and sequential measurements should be used, in conjunction with hepatic function tests and biopsies, to ascertain a prognosis.
Albumin is synthesised in the liver, usually at only 33% of the maximum capacity. The half life of albumin is 8-9 days, so disturbances in serum albumin levels only occur in chronic hepatobiliary disease.
Bile acids are also synthesised by the liver from cholesterol, they are then excreted into bile and stored in the gallbladder. Bile acids are transported back into the portal circulation from the ileum. Any disruption in this enterohepatic circulation of bile acids will result in increases in serum levels. Bile acid stimulation tests involve taking a blood sample after a 12 hour starve, then again 2 hours after a meal. The bile acid stimulation test is both more sensitive and specific for detecting hepatobiliary disease.

Abdominal radiography can be used to assess size and opacity of the liver. Hepatomegaly will result in caudal displacement of the stomach and extension of the hepatic shadow beyond the costal arch. Hepatomegaly can be due to:
- Congestion
- Infiltrative disease (neoplasia, lipidosis, glycogen accumulation, amyloidosis)
- Inflammatory disease
- Extramedullary haematopoiesis
Focal hepatomegaly can be seen with cysts, granulomas, abscess, haematomas or neoplasia. Microhepatica will have a reduced hepatic shadow, with cranial displacement of the stomach and the gastric axis being more upright. This can be observed with hepatic atrophy, cirrhosis and PSS.
Ultrasonography allows differentiation between diffuse and focal hepatic disease. It also allows assessment of hepatic parenchyma, the biliary system and portal vasculature. Diffuse disease in the liver can be classified as hyperechoic or hypoechoic.
Hyperechoic: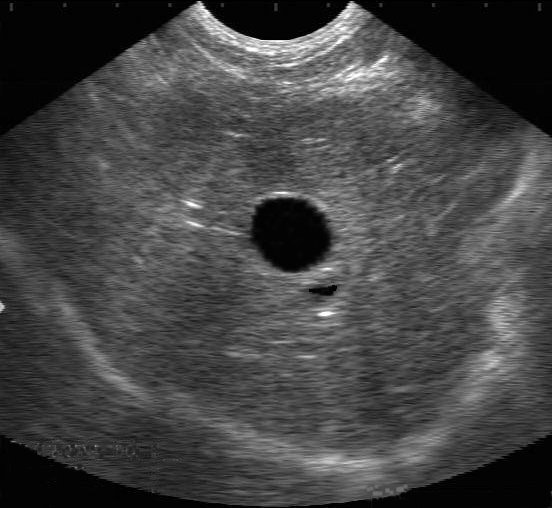
- Fibrosis
- Lipidosis
- Corticosteroid hepatopathy
- Hepatic neoplasia (lymphoma, bile duct adenocarcinoma)
Hypoechoic:
- Suppurative hepatic disease
- Passive congestion
- Hepatic lymphoma
The collection of a liver biopsy for cytological or histopathological evaluation is often necessary for a definitive diagnosis. This biopsy can be obtained by ultrasound-guided needle biopsy, laprascopic biopsy or wedge biopsy by laparotomy. The biopsy should be able to categorise the disease (necroinflammatory, neoplastic, vacuolar or vascular), the severity (mild, moderate or severe) and the chronicity of the disease (presence of fibrosis, type of inflammatory cells present). As there is often an associated coagulopathy and haemorrhage is the main complication associated with obtaining a liver biopsy, the patient’s PT, APTT and platelet count should be assessed. Due to the high frequency of vitamin K deficiency in hepatic disease and the ease with which it is treated, many clinicians routinely pre-treat all patients with parenteral vitamin K1 24 hours prior to hepatic biopsy.
Classification of liver disease
Due to the liver’s central role in body function, it is exposed to many “threats.”
Secondary hepatopathies usually result in vacuolation of the hepatocyte, this can be due to:
- Right-sided congestive heart failure
- Hypoxia
- Anaemia
- Shock
- Glucocorticoids
- Endogenous (HAC)
- Exogenous (steroid therapy)
- Diabetes mellitus
- Hyperlipidaemia (e.g. Schnauzers)
- Hyperthyroidism
- Hypothyroidism
- Non-hepatic inflammatory disease
- Toxaemia
- Sepsis
- GI disease
- Pancreatitis
- Drug-induced
- Phenobarbitone
- Steroids
It is also worth mentioning Triaditis as a disease entity. This is the development of concurrent inflammatory bowel disease, pancreatitis and biliary tract disease. This occurs because unlike the dog, the cat’s pancreatitic duct enters the common bile duct before it opens into the duodenum. When there is disease (e.g. infection, inflammation, and neoplasia) in the small bowel, it may ascend into the common bile duct and, from there; affect the pancreas and the rest of the biliary tree. Similarly, disease in the biliary tree or pancreas may affect the other two regions.
Treatment
Therapeutic intervention should be as early as possible to try to stop fibrosis and cirrhosis. Therapy is, in most cases, supportive and non-specific.
Glucocorticoids – Most used therapy for chronic hepatitis. They have anti-inflammatory effects, but also have anti-fibrotic and cholerectic effects. They are contraindicated if any infectious cause is diagnosed. DO NOT use steroids in end stage cirrhosis or non-inflammatory fibrosis or dogs with significant portal hypertension.
Azathioprine – If additional immunosurpressive action is required. For use in dogs only.
Antibiotics – If suppurative hepatitis is diagnosed, choice of antibiotic should be based on culture and sensitivity.
Ursodeoxycholic Acid (UDCA) – UDCA is one of the natural bile acids in the enterohepatic circulation. As UDCA is hydrophilic it is a non-toxic bile acid, the less hydrophilic bile acids tend to be highly toxic especially in the liver where they are concentrated. Toxic bile acids will induce hepatocyte apoptosis and cause free radical formation which leads to oxidative damage to cells. UDCA is thought to increase bile acid flow, dilute out the toxic bile acids and modulate the immune system (especially useful in cases where autoimmune disease is suspected). UDCA, as a bile acid, can be picked up on measurement of serum bile acids, so clinicians may notice an increase in serum bile acids after starting treatment, which would not indicate a deterioration in liver function. UDCA is contraindicated in cases of extrahepatic bile duct obstruction.
S-Adenosyl-L-methionine (SAMe) – Glutathione (GSH) is one of the main defence mechanism of the hepatocyte against intoxication, and depletion of GSH causes oxidative stress. SAMe is a precursor of cysteine, which is one of the amino acids of GSH. SAMe is important in the defence against free radicals. Must be given on empty stomach.
Silymarin – Silymarin is the active component extracted from the fruit of Silybum marianum, milk thistle. Silybin is the most active component of Silymarin. Silybin appears to be a strong free radical scavenger by increasing intracellular levels of superoxide dismutase (SOD).
Demarain and Denamarin Chewable are available in the UK. They provide a quality source of SAMe and Silybin, with proven bioavailability and hepatoprotective effects on hepatocytes.
Antifibrotics – The end-stage of all chronic hepatic disorders, if inadequately treated, is fibrosis. Once fibrosis has occurred the process is irreversible and no regeneration is possible. Colchicine is the only drug used specifically to stop and reduce fibrosis, it is thought to act via stimulation of the collagenase activity. It has been known to cause vomiting and diarrhoea.
Diet – Palatable diet of high biological value protein, decreased sodium, increased vitamin K and zinc. Should be fed little and often (4-6 times per day). DO NOT RESTRICT PROTEIN unless necessary to control hepatic encephalopathy.
In human medicine, single agent therapy has proven less effective than polymodal approaches in the treatment of liver disease.
Oxidative Stress...
Free radicals or reactive oxygen species are molecules that have one or more unpaired electrons. Because they are unstable and highly reactive, they try to capture the needed electron(s) from other molecules. When this happens, the other molecule itself becomes a free radical, beginning a chain reaction. Free radicals cause damage to membranes, organelles and cells as molecules lose their full complement of electrons. Free radicals are generated where there is inflammation and infection, but also certain drugs and minerals (e.g. copper) produce them.
Conditions associated with oxidative stress:

... and antioxidants
The term anti-oxidant refers to many substances that have the ability to neutralise free radicals, usually by donating an oxygen or hydrogen electron. Deactivating free radicals stops cellular and tissue damage. Antioxidants may also act by scavenging free radicals, preventing further free radical formation. In health, there is a balance between free radical levels and antioxidant production, if the balance tips in the favour of free radicals, oxidative stress and cell damage occur. There are many members of the antioxidant defence system, including those the body makes, as well as nutritional and supplementation agents.
Antioxidants should be considered in all cases of liver disease.
Glutathione
Glutathione is involved in several antioxidant pathways in the liver and is probably the most important antioxidant providing a vital hepatic defence mechanism. It is a transpeptide of cysteine, glycine and glutamate. Mitochondrial glutathione depletion occurs as an early event in many forms of toxic liver injury and sensitises hepatocytes to cell death. It is not possible to supplement glutathione directly, it is poorly absorbed from the gut, and as a result supplements aim to increase hepatocyte production.
S-Adenosyl-L-methionine (SAMe)
SAMe is synthesised by all cells, it is derived from methionine (an amino acid) and ATP, under the action of the enzyme SAMe synthetase. SAMe initiates 3 major biochemical pathways:

SAMe is a naturally occurring molecule that is vital in the production of Glutathione, the main hepatic anti-oxidant. The production of SAMe is decreased with hepatic injury, resulting in decreased Glutathione levels and thus promoting oxidative damage. This occurs due to the down-regulation of the enzyme, SAMe synthetase, which is vital for the conversion of methionine and ATP into SAMe.
SAMe benefits/effects:

Better absorption of SAMe is achieved when fed on an empty stomach at least an hour before food. SAMe is also very susceptible to breakdown by the stomach acid so products should be enteric coated. There are 2 isomers of SAMe known as the S, S isomer (biologically active form) and the R, S isomer (biologically inactive, may actually impair biologic utilization of the active S, S isomer). In most hepatic support products the relative amounts of the S, S isomer and R, S isomer is 50:50 (75:25 in Denamarin, due to unique production process), if the product is exposed to the environment, moisture or stomach acid then the S, S isomer is converted to the inactive R, S isomer. This process can be detected by the clinician as a sulphurous smell (rotten eggs) is given off!
Silybin
- Beneficial effects attributed to:
- Direct antioxidant activity
- Stops lipid peroxidation (deterioration of lipids due to oxidation)
- Enhanced detoxification of toxins
- Thiol substrate donation (helps in GSH recycling)
- Anti-inflammatory and immunomodulatory effects
- Stimulation of cell repair
Vitamin E
Lipid-soluble antioxidant. Mitochondria and Kupffer cells accumulate vitamin E to help with protection of the cells. It is often referred to as the “last line of defence against lipid peroxidation.” When vitamin E is oxidised it becomes a free radical and potentially harmful if not converted back to its original form, this is achieved by vitamin C.
Zinc
Essential co-factor involved in many biological reactions. It helps reduce heavy metal absorption in disease states such as copper storage disease. It is also said to have anti-fibrotic properties and be hepatoprotective, by inhibiting lipid peroxidation and stabilising membranes.
Vitamin C
Water-soluble reducing agent. Able to convert Vitamin E back to active form. Should be avoided where issues with copper storage (e.g. some chronic hepatopathies and copper storage disease of Bedlington terriers) as it may enhance transition metal oxidative injury.
This article was brought to you by Protexin - makers of Denamarin & Denamarin chewable.


