Show all small animal articles
Your First Fracture Repair: Principles and Planning in Practice
Hannah Gritti MRCVS, British Veterinary Orthopaedic Association. - 09/07/2021

Your First Fracture Repair: Principles and Planning in Practice
Hannah Gritti, British Veterinary Orthopaedic Association
If this Ten Minute Top-Up has caught your eye, then check out the BVOA website for details of courses, discussion groups and more...
For more details follow the link to the BVOA website below.
When repairing a fracture,the main aims are to achieve alignment, optimal healing environment and the avoidance of fracture disease which includes muscle atrophy/contracture, joint stiffness and disuse osteoporosis and therefore in suboptimal limb function. So how do you translate this in practice? The following considerations are appropriate for a diaphyseal shaft fracture of e.g. the femur.
Principles of Fracture Management
Consider mechanical stability and fracture biology.
Bone healing relies on:
1. Stability
Stabilising the fracture can reduce the risk of further damage, provide analgesia, and control soft tissue swelling.
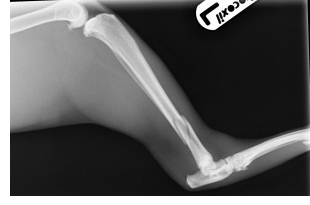
Orthogonal radiographs of the fractured bone should be taken, and usually also the contralateral limb. Careful inspection of the images will help to detect fragments, fissures and other potential complicating factors. The ability to measure the bone and pre-contour bone plates is invaluable so use a scale marker and implant templates (digital or acetates). Have the radiographs available during surgery for immediate reference.
Choose between either open reduction and internal fixation (ORIF) or closed reduction for example with an ESF. Implant selection is based on awareness of forces around a fracture. Consider patient size, temperament and muscle mass when considering implant selection, and have a back-up plan if your first choice becomes unsuitable during surgery.
Implants:
- Bone plates (Fig.1.)
− Non-locking (e.g., dynamic compression plate [DCP], limited contact DCP)
These plates must have good bone apposition along the length of the plate and require perfect contouring. They can be applied in bridging, neutralisation or compression mode depending on the type of fracture e.g. a dynamic compression plate is used to compress a transverse fracture.
− Locking plates (e.g., locking compression plate [LCP] or string-of-pearl [SOP])
The screw heads lock into the plate. The plate is not pressed down onto the bone therefore the plate and bone do not have to be in direct contact; only approximate contouring is required.
- Screws - self-tapping or not, cortical or cancellous. Can be used to secure plates or in a lag fashion in combination with other fixation techniques. A lag screw engages the far (trans) cortex but not the near (cis) cortex and can be full or partially threaded. It must be placed perpendicular to the fracture line and applies compression across the fracture.
- Plate/rod combinations - provide more resistance to bending and are very useful when used in combination with bridging plates.
- External skeletal fixators (Fig.9)
- Additional implants such as wire or pins (Fig.10 & 11)
2.Reduction
Are you aiming for primary or secondary bone healing and is anatomical reconstruction appropriate? Reconstruction is more difficult with comminuted fractures with many free fragments that if devascularised, may significantly delay bone healing or result in non union. It is possible to leave fragments undisturbed with bridging plates where the plate bears the entire load (forces) across a fracture gap. There must be sufficient bone stock proximal and distal to the fracture to insert two or three bicortical screws as a minimum, and ideally more.
The ease of reduction is affected by time to surgery, muscle contracture and operative technique. If possible use the ‘hanging limb’ technique i.e. using the animal’s bodyweight to distract to the fracture whilst suspended during preparation pre-operatively. Also use an assistant and/or retractors. Positioning the limb parallel to the table helps with angulation of the drill and implants and is appropriate for a medial or lateral approach. Secure the patient on the table and use positioning aids.
3.Prevention of infection
Good preparation and planning will minimise the length of surgery.
Ensure aseptic technique for the fracture, bone graft and local block sites. If using the hanging limb technique, ensure that an assistant can hold the leg whilst you drape the area, and use sterile bandage or smaller drapes to isolate the foot, without contaminating your incision site.
Good haemostasis including the use of swabs, haemostats and electrocautery is one of Halsted’s principles of surgery and is one factor that will help to reduce the incidence of post-operative surgical site infection.
Use antibiotic prophylaxis if necessary but ensure that adequate concentrations of antibiotic are present in advance of the first incision i.e. give the first dose at the time of pre-med or anaesthetic induction.
4.Preservation of blood supply.
Know the anatomy and surgical approach to your fracture site; this will depend on soft tissue cover, any wounds and accessing the tension surface of the bone rather than the compression (bending) surface. Employ Halsted’s principles of surgery including sharp dissection between muscle and fascial planes. Minimum disturbance of the fracture haematoma, vessels and soft tissues is favourable for healing. Keep tissues moist with sterile saline irrigation.
5.Encouraging limb use
Plan your approach to avoid iatrogenic nerve damage, achieve good fracture alignment and provide adequate analgesia for a fast return to function post-op.
Planning the Repair
Check you have everything you need and that it will be sterilised in time for surgery.
Orthopaedic Kit
1.Plates and screws kit:
- Plate types- dynamic compression , T-plate
- Screw in 2 sizes

Fig. 1:
2.Retractors:
- Hohman (left)
- Gelpi self-retaining retractors
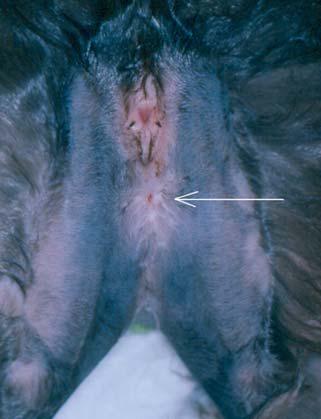
Fig. 2
3.Jacob’s Chuck with key and extensions for use with long pins and the drill.

Fig. 3
4. Drill:
- a variety of drill bits are necessary to be used with different screw sizes.

Fig. 4
5. Drill guide:
- This is for a 2.0mm dynamic compression plate, and fits into the oval holes to direct the drill in neutral or compression positions.

Fig. 5
6. Depth gauge:
- Having a range of sizes is helpful, this is used to measure the depth of hole in the bone so that the correct length of screw can be used.

Fig. 6
7. Tap with tap handle:
- This is used to cut a thread in the bone prior to insertion of a non self-tapping screw.
- A tap is not required for a self-tapping screws that cut their own thread.
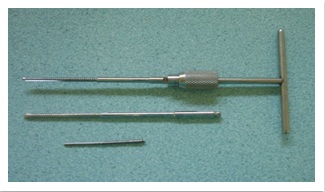
Fig. 7
8. Pin cutter:
- This is used to cut K-wires, pins and orthopaedic wire.
- Do not use the pin cutter on a size of wire greater than the maximum stated on the pin cutter.

Fig. 8
9. Plate Benders:

Fig. 9
10. ESF kit:
- Connecting bars
- Clamp
- Can have a variety of different set-ups classified as such

Fig. 10
11.Wire and wire benders/cutters:
- Wire of varying diameters can be used in a cerclage or figure-of-eight fashion
- K-wire is in fact Kirschner wire which refers to pins of 2.0mm diameter or less.
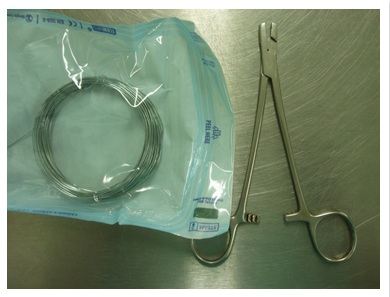
Fig. 11
12. Pins:
- Pins can be used in an intramedullary fashion with retrograde or normograde placement (the former directs the pin up the medullary cavity via the fracture).
- Steinmann (intramedullary) pins are defined as over 2.0mm in diameter and can be threaded or smooth.
- Kirschner wire is a smaller diameter pin used to immobilise small bone fragments, as an anchor for figure-of-eight wire or as a temporary stabiliser before a plate is applied.
- A smaller size diameter IM pin will make placing a plate in combination easier as it allows more space for the screws to pass; a size that equals 30-50% the medullary canal diameter is advised when used as a plate-rod.

Fig. 12
13. Drill sleeve:
- Used to protect soft tissues and prevent the drill bit from skidding when drilling a hole.
- Two different drill bits are needed to place a lag screw. The cis cortex is drilled first, a drill sleeve is inserted into the hole then the trans cortex is drilled with a smaller diameter drill bit. The lag screws engages the far cortex but not the near (cis) cortex so that the head of the screw applies compression. This is used to stabilise and achieve primary bone union across an oblique fracture.

Fig. 13
Further Reading
- Coughlan A, Miller A (Eds). BSAVA Manual of Small Animal Fracture Repair and Management. Second Edition. 2006. BSAVA.
- Piermattei DL, Flo GL, DeCamp CE. Handbook of Small Animal Orthopaedics and Fracture Repair. Fourth Edition. 2006. Saunders Elsevier.

