Lameness in sheep flocks
Lindsay Rochford BVM&S MRCVS - 19/03/2011
Lameness in sheep flocks
Lameness is known to be one of the most important welfare issues affecting the UK sheep industry. It is estimated that over 80% of flocks contain lame sheep (Winters 2004). There are many causes of lameness, and these causes must be determined in order to instigate effective treatment. A lame sheep does not necessarily mean footrot! As vets we may be asked to examine individual lame sheep or flock problems. Any lame sheep should be a concern, however when dealing with flocks it is practical to set an intervention level and this has been suggested to be 5% prevalence (Winters 2004). Flocks that have prevalence higher than this should be investigated immediately.
Examination in order to reach a diagnosis
It must be remembered that the clinical picture will vary depending on the stage of the disease and that sometimes it can be difficult to determine what disease is present eg) the end stage of footrot vs. severe white line degeneration. Below is a re-cap on the important and distinguishing features of the common conditions causing foot lameness in sheep...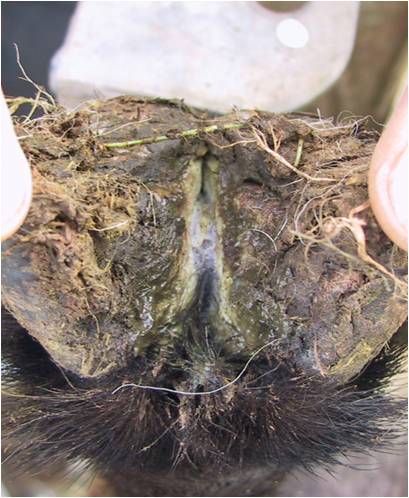
Scald/Interdigital Dermatitis
- Fusobacterium necrophorum
- Affects the interdigital space only
- Characteristic appearance: reddening and slight swelling of the interdigital skin, damp looking, loss of hair
- High percentage of animals affected
Footrot
- Fusobacterium necrophorum plus Dichelobacter nodosus
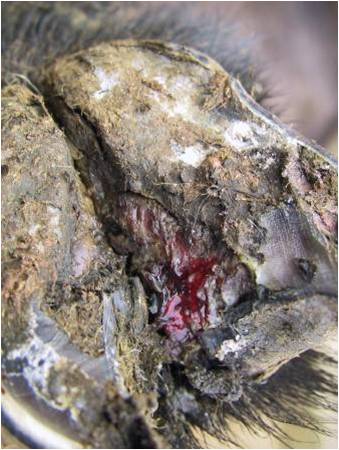 Fusobacterium necrophorum causes damage to the interdigital skin (as seen with scald/interdigital dermatitis), this allows penetration of the deeper structures of the hoof by its partner in crime Dichelobacter nodosus
Fusobacterium necrophorum causes damage to the interdigital skin (as seen with scald/interdigital dermatitis), this allows penetration of the deeper structures of the hoof by its partner in crime Dichelobacter nodosus- Dichelobacter nodosus...

- produces the enzymes protease and elastase which cause separation of the hoof from the underlying structures
- characteristic foul smell
- 10 different strains of Dichelobacter nodosus of varying virulence. A mix of strains may be present.
- Benign footrot – very little separation and under running
- Virulent footrot –complete separation
- can survive in animals feet for prolonged periods
- can survive on pasture for up to 14 days
Contagious ovine digital dermatitis (CODD)
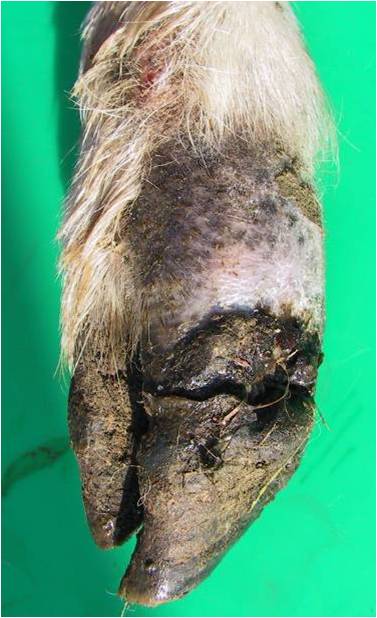 First reported in 1997
First reported in 1997- Characteristic appearance: Primary lesion at the coronary band, rapid invasion and under running of the hoof wall from the coronary band downwards
- Results in complete shedding of the hoof capsule. In severe cases the regrowth of horn can be permanently affected
White line degeneration (shelly hoof)
- Partial detachment of the hoof wall and subsequent impaction of soil
- Formation of pus under the wall
- Released by paring, if not...
- Tracks up to the coronary band and after a few days bursts out and discharges
- Aetiology thought to be nutritional
White line abscess
- Also a result of a defect to the white line
- However less obvious presentation than seen with white line degeneration
- Sudden onset, severe lameness
- Pain and heat in claw
- Paring reveals dark mark/s, on further paring pus will be released, as with white line degeneration can track up to coronary band and burst out
Pedal joint sepsis
- Claw acutely painful and swollen, bursting out of pus at several points around the coronary band, loss of hair at coronary band
- No resolution following discharge of pus
- Severe lameness, remains swollen and horn appears defective
- Deep digital flexor tendon may rupture – classically seen as the toe pointing upwards
- Infection usually remains localised to the hoof – unlikely to see tracking of infection up the tendon sheath
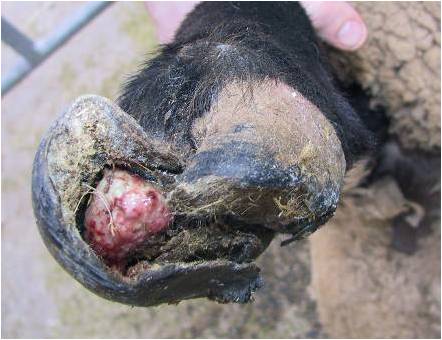
Granuloma
- Classical appearance: strawberry like growths
- Mostly found at the toe
- Due to over paring
- Can occur secondary to trauma or footrot
Treatment
Foot paring
Care must be taken to ensure paring is not carried out excessively. Paring should be used to help find the source of a problem and provide a diagnosis, to remove loose horn and to remove overgrown horn. Excessive and over-zealous paring can result in bleeding and subsequent formation of toe granulomas.
Footbaths
Footbaths must be well maintained. Gold standard would be to have 2 footbaths, one with water to clean the feet followed by the footbath with the chemical added. It is advised sheep stand on hard ground for 30 minutes post bathing.
Formalin
- 2-3% solution
- Excessive strength or repeated use can cause hardening and cracking of the hooves
- It is denatured by organic material – therefore requires changed when it becomes contaminated with mud and faeces
Zinc sulphate
- 10% solution
- Remains active in the presence of organic material
- Sheep must stand in the footbath for a period of time (check guidelines for specific product)
Antibiotics
- No antibiotic is licensed for the use in footbaths
- Lincomycin/spectinomycin and tylosin soluble powders have been used
- Standard withdrawal periods must be adhered to
Topical sprays
- Most commonly used is oxytetracycline
- Effective in cases of scald and early footrot
- After treatment confine to a dry standing area for at least 30 minutes
- Animals treated with a spray should not be additionally footbathed
Antibiotic injections
- Particularly useful for virulent footrot and individual cases of infectious lameness
- Long acting oxytetracycline, a penicillin/streptomycin combination and tilmicosin (Micotil) have all been used with success for treating footrot (Winters 2004)
- In cases of CODD, tilmicosin (Micotil) has been found to be very effective (Watson 1999)
Vaccination
Only effective for the control of footrot
It doesn’t end there...
It is important to note that the consequences of lameness don’t stop at the clinical signs. It can have a knock on effect to fertility, body condition and can predispose to other diseases. Rams which are lame at tupping time will tend to mate with fewer ewes, leading to lower conception rates. Lameness in ewes can result in the birth of lower weight lambs than expected, poor quality colostrum and reduced milk production. Infectious lameness in ewes after lambing is likely to spread to the lambs, reducing growth rates and therefore delaying time to finishing.
This article was kindly provided by Elanco Animal Health, makers of Micotil:

References
Watson C.L. (1999) Severe foot lesions in sheep, Letter, Veterinary Record, 145, 711
Winters A (2004) Lameness in sheep 1. Diagnosis, In Practice, 26 ,58-63
Winters A (2004) Lameness in sheep 2. Treatment and Control, In Practice, 26, 130-139

